Glaucoma Fact Sheet
What Is Glaucoma?
Glaucoma is a group of eye conditions that damage the optic nerve. The optic nerve sends visual information from your eye to your brain and is vital for good vision. Damage to the optic nerve is often related to high pressure in your eye, but glaucoma can happen even with normal eye pressure.
Glaucoma can occur at any age but is more common in older adults. It is one of the leading causes of blindness for people over the age of 60.
What Causes Glaucoma?
Glaucoma develops when the optic nerve becomes damaged. As this nerve gradually deteriorates, blind spots develop in your vision. For reasons that doctors don’t fully understand, this nerve damage is usually related to increased pressure in the eye.
Elevated eye pressure happens as the result of a buildup of fluid, called aqueous humor, that flows throughout the inside of the eye. It usually drains through a tissue, called the trabecular meshwork, located at the angle where the iris and cornea meet. When the eye makes too much fluid or the drainage system doesn’t work properly, eye pressure may increase.
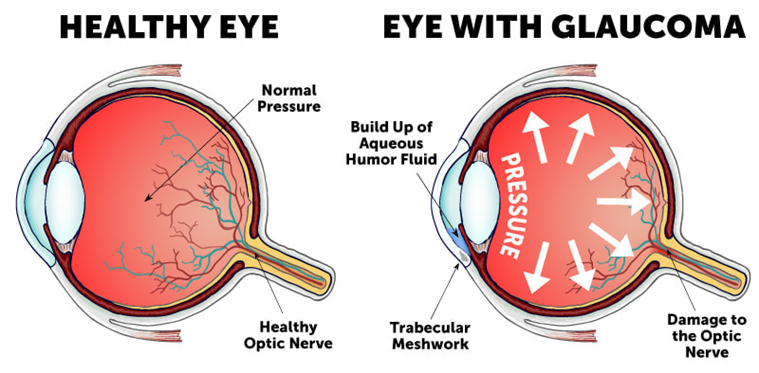
Image courtesy of Wolfe Eye Clinic
What Are the Types of Glaucoma?
There are several types of glaucoma, including:
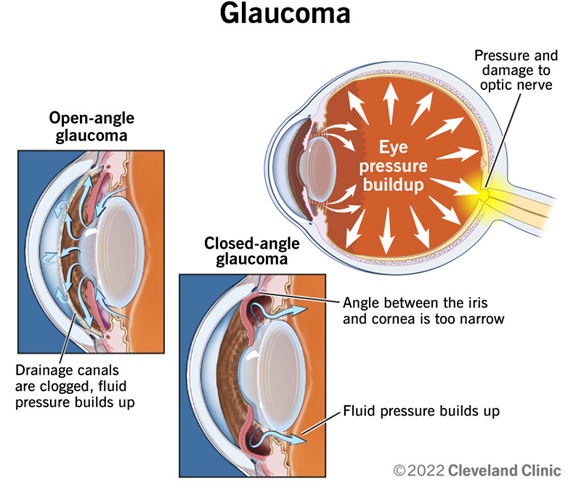
Open-Angle Glaucoma
This type is the most common, affecting up to 90% of Americans who have glaucoma. It occurs when resistance builds up in your eye’s drainage canals. Over months or years, the fluid in your eye can build up and put pressure on your optic nerve. The disease may go unnoticed for years because most people don’t have symptoms.
Closed-Angle Glaucoma
Also called angle-closure or narrow-angle glaucoma, this rare type often comes on suddenly (acute). It occurs when the angle between your iris and cornea is too narrow. It may happen when your pupil changes and becomes too big (dilated) too quickly. This blocks your drainage canals and prevents aqueous fluid from leaving your eye, causing eye pressure to rise. Symptoms, including eye pain and headaches, can be severe and require immediate medical attention.

Normal-Tension Glaucoma
As many as 1 in 3 people have optic nerve damage even when eye pressure is normal or not very high. Experts are uncertain about what causes normal-tension glaucoma. The optic nerve may be sensitive or experience less blood flow. Another name for this type is normal-pressure or low-tension glaucoma. This type is more common among people of Asian descent or Asian Americans.
Congenital Glaucoma
Some babies are born with drainage canals that don’t form properly in the womb. Your healthcare provider might notice your baby’s glaucoma symptoms at birth or signs may become noticeable during childhood. Other names for this type are childhood, infantile or pediatric glaucoma.
What Are the Symptoms of Glaucoma?
For some types of glaucoma, there aren’t any early warning symptoms, and changes to vision can happen gradually, so the symptoms are easy to miss. Because many people with open-angle glaucoma don’t have any noticeable symptoms, it’s very important to have routine eye exams to detect this disease in its earlier stages. Glaucoma damage is irreversible, so you need early detection and treatment to prevent blindness.
Closed-angle glaucoma has more severe symptoms that tend to come on suddenly.
With any type, you may experience:
- Eye pain or pressure
- Headaches
- Rainbow-colored halos around lights
- Low vision, blurred vision, narrowed vision (tunnel vision) or blind spots
- Nausea and vomiting
- Red eyes
What Are Risk Factors for Glaucoma?
Glaucoma can affect anyone, but the risk increases with age. People who are Black and Hispanic are much more likely to get glaucoma than other ethnic groups, and they tend to develop the disease earlier in life. Asian and Inuit populations are also more susceptible to a specific form of glaucoma known as angle-closure glaucoma or closed-angle glaucoma.
People with diabetes are twice as likely to get glaucoma. Other risk factors include:
- Family history of glaucoma
- Farsightedness or hyperopia (for closed-angle glaucoma)
- High blood pressure (hypertension) and very low blood pressure (hypotension)
- Long-term use of corticosteroids, especially eye drops
- Nearsightedness or myopia (for open-angle glaucoma)
- Previous eye injury or surgery
- History of migraines, high blood pressure, or sickle cell anemia
- High internal eye pressure, also known as intraocular pressure
- Corneas that are thin in the center
How Is Glaucoma Diagnosed?
Your health care provider will review your medical history and conduct a comprehensive eye examination. Your provider may perform several tests, including:
- Measuring intraocular pressure with tonometry
- Testing for optic nerve damage with a dilated eye examination, to widen pupils and view your optic nerve, and imaging tests such as a slit-lamp exam or optical coherence tomography (OCT)
- Checking for changes in peripheral vision (your ability to see off side) with a visual field test, also known as perimetry
- Measuring corneal thickness with an exam called pachymetry
- Inspecting the drainage angle, also known as gonioscopy
- Visual acuity test (eye charts) to test for vision loss
How Is Glaucoma Treated?
Untreated glaucoma can lead to faster development of permanent vision loss or blindness. Treatments can slow down additional vision loss, but they can’t restore lost vision. It’s important to see an eye doctor right away if you have eye pain, severe headaches or vision problems.
Medications to Treat Glaucoma
Glaucoma treatment often starts with prescription eye drops. Some decrease eye pressure by improving how fluid drains from your eye. Others decrease the amount of fluid your eye makes. Depending on how low your eye pressure needs to be, you may be prescribed more than one eye drop. Because glaucoma is a lifelong condition, you may need to use daily eye drops for life. You may have to apply them more than once a day. There are many types of prescription eye drops, including prostaglandins, beta blockers, alpha-adrenergic agonists, carbonic anhydrase inhibitors, rho kinase inhibitors, and mitotic or cholinergic agents.
The U.S. Food and Drug Administration (FDA) has approved two new delivery devices for implants that continuously deliver eye drop medications. Durysta® is an implant for bimatoprost, a glaucoma treatment that’s been available as eye drops. It dissolves and works for six months. Currently, you can only have it placed once in each eye. The other implant, iDose TR, is a first-of-its kind treatment that is designed to provide up to three years of 24/7, continuous drug therapy directly inside the eye. This implant delivers the drug travaprost. Both implants are placed in your eye by your eye doctor.
Eye drops alone may not bring your eye pressure down to the desired level, so your eye doctor may also prescribe oral medicine. This medicine is usually a carbonic anhydrase inhibitor.
Laser Therapy to Treat Glaucoma
Your eye doctor may use a laser (a strong beam of light) to help improve fluid drainage from your eye in a procedure called laser trabeculoplasty (truh-BEK-u-low-plas-tee). Your provider may suggest lasers as a first-line therapy instead of drops or in addition to eye drops. Having laser treatment may not replace the use of eye drops completely. The results from laser treatments vary but can last for years in some cases. Your provider may be able to repeat some types of laser treatments. The treatment can be done in your eye doctor’s office.
Surgery to Treat Glaucoma
Surgery is another way to help reduce eye pressure. It’s more invasive but can also achieve better eye pressure control faster than drops or lasers. Surgery can help slow down vision loss, but it can’t restore lost vision or cure glaucoma. There are many types of surgeries for glaucoma, and depending on the specific type and severity, your eye doctor may choose one over another. Types of surgery include:
- Filtering surgery. This is a surgical procedure called a trabeculectomy (truh-bek-u-LEK-tuh-me). The eye surgeon creates an opening in the white of the eye, which also is known as the sclera. The surgery creates another space for fluid to leave the eye.
- Drainage tubes. In this procedure, the eye surgeon inserts a small tube in your eye to drain excess fluid to lower eye pressure.
- Minimally invasive glaucoma surgery (MIGS). Your eye doctor may suggest a MIGS procedure to lower your eye pressure. These procedures generally require less immediate postoperative care and have less risk than trabeculectomy or using a drainage device. They are often combined with cataract surgery. There are a number of MIGS techniques available, and your eye doctor will discuss which procedure may be right for you.
After your procedure, you’ll need to see your eye doctor for follow-up exams. You may eventually need to undergo additional procedures if your eye pressure begins to rise or other changes occur in your eye.
Treating Angle-Closure Glaucoma
Acute angle-closure glaucoma is a medical emergency. If you’re diagnosed with this condition, you’ll need urgent treatment to reduce the pressure in your eye. This generally will require treatment with medicine and laser or surgical procedures. You may have a procedure called a laser peripheral iridotomy. The doctor creates a small hole in your iris using a laser. This allows fluid to flow through the iris. This helps to open the drainage angle of the eye and relieves eye pressure.
What Does the Future Hold for Glaucoma Treatment?
1. Glaucoma destroys retinal ganglion cells, nerve cells that receive visual information from light-sensing photoreceptors and transmit it to the brain, resulting in vision loss. A multi-disciplinary team led by researchers at the Schepens Eye Research Institute of Mass Eye and Ear has found a promising new strategy for retinal ganglion cell replacement. They changed the microenvironment in the eye in a way that enabled them to take stem cells from blood and turn them into retinal ganglion cells that could migrate and survive in the eye’s retina. The team conducted their study on the adult mouse retina, but the method could one day be applied to human retinas.
2. The trabecular meshwork (TM) is the spongy tissue located near the cornea through which aqueous humor flows out of the eye. TM fibrosis increases resistance to this outflow and is a crucial pathophysiological process in the development of primary open-angle glaucoma. Pirfenidone (PFD) is a new, broad-spectrum antifibrotic agent approved for the treatment of idiopathic pulmonary fibrosis, a condition in which the lungs become scarred and breathing becomes increasingly difficult. A study using cultured human TM cells and a mouse model of ocular hypertension suggests that pirfenidone may also be useful in inhibiting TM fibrosis and improving intraocular pressure in glaucoma patients.
3. Inside our eyes, we have a natural lens that bends light rays that come into the eye to help us see. When the lens becomes cloudy due to cataracts, it may be surgically replaced by an artificial lens known as an intraocular lens. SpyGlass Pharma is developing an intraocular lens that is embedded with a drug delivery platform to continuously deliver the glaucoma drug bimatoprost over multiple years. The lens is designed to be implanted at the time of cataract surgery. The company announced the initiation of a Phase I/II clinical trial investigating the platform in patients with glaucoma and cataracts in October.
Sources:
Mayo Clinic Staff. “Glaucoma-Symptoms and Causes” and “Glaucoma-Diagnosis and Treatment.” Mayo Clinic, 30 Sep. 2022, www.mayoclinic.org/diseases-conditions/glaucoma/diagnosis-treatment/drc-20372846
“Glaucoma.” Cleveland Clinic, 18 Nov. 2022, https://my.clevelandclinic.org/health/diseases/4212-glaucoma
National Glaucoma Research. “FDA Approves First-of-its-Kind Glaucoma Treatment.” Bright Focus Foundation, 15 Dec. 2023, https://www.brightfocus.org/glaucoma/news/fda-approves-first-its-kind-glaucoma-treatment
Massachusetts Eye and Ear Infirmary. “Researchers develop potential glaucoma treatment strategy to guide stem cells to the retina.” Medical Xpress, 18 Nov. 2023, https://medicalxpress.com/news/2023-11-potential-glaucoma-treatment-strategy-stem.html
Compiled/edited by M. Kaplan, PhD, 5/2024
Information Disclaimer: We do not recommend any particular treatment. Our Material might not represent all that is available on the subject. This information might not apply specifically to your own condition. Our Material is not intended as a substitute for medical care. Our Material should be used to formulate questions for discussion with your physician. We hope that the information you find at The Health Library will be useful in communicating with your health professionals. If you have any questions about your unique medical condition, we strongly advise that you see your physician.
