Age-Related Macular Degeneration (AMD) Fact Sheet
What is Age-Related Macular Degeneration (AMD)?
Age-related macular degeneration (AMD) is a problem with your retina, the light-sensing nerve tissue at the back of the eye. It happens when the centermost part of the retina, called the macula, is damaged. With AMD you lose your central vision. You cannot see fine details, whether you are looking at something close or far. But your peripheral (side) vision will still be normal. For instance, imagine you are looking at a clock with hands. With AMD, you might see the clock’s numbers but not the hands.
AMD is very common. It is a leading cause of vision loss in people 50 years or older. Many people don’t realize they have AMD until their vision is very blurry. This is why it is important to have regular visits to an ophthalmologist. He or she can look for early signs of AMD before you have any vision problems.
What are the two types of AMD?
There are two types of AMD, dry AMD and wet AMD.
Dry AMD
About 90% of people who have AMD have the dry form. Dry AMD is when parts of the macula get thinner with age and tiny yellow deposits made up of lipids (fats) and protein, called drusen, grow. With dry AMD, you slowly lose central vision.
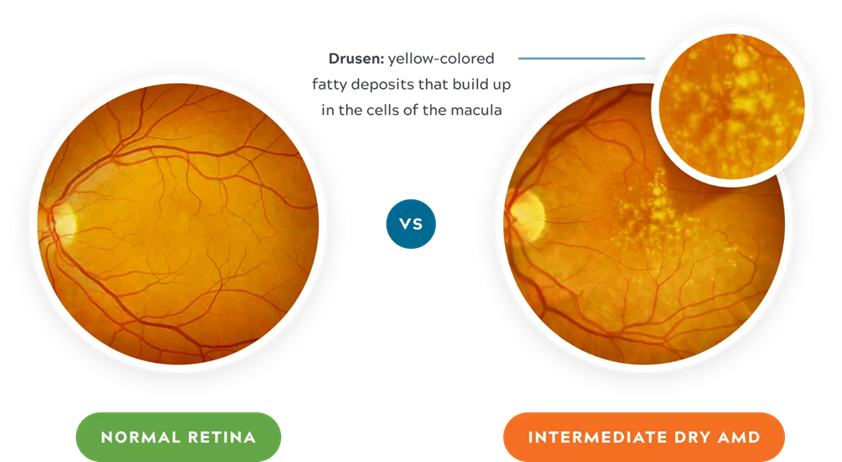
Image Courtesy of Foresee Home
Comparison of a normal retina vs a retina with dry AMD
The last stage of dry AMD is called geographic atrophy, which causes regions of cells in the retina to waste away and die resulting in a growing blind spot in the visual field. This makes it difficult to drive, read, and even recognize faces. Up to 20% of people with AMD develop geographic atrophy.
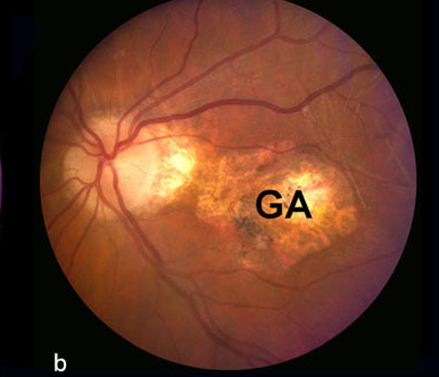
Picture of an eye with geographic atrophy (GA)
Image courtesy of Webvision
While geographic atrophy is more commonly associated with the dry subtype of AMD, it is possible for people to have both wet and dry AMD at the same time, and to develop geographic atrophy independently of having wet AMD.
Wet AMD
Wet AMD is less common but much more serious. Wet AMD is when new, abnormal blood vessels grow under the retina. These vessels may leak blood or other fluids, causing scarring of the macula. You lose vision faster with wet AMD than with dry AMD. Dry AMD can turn into the wet form.
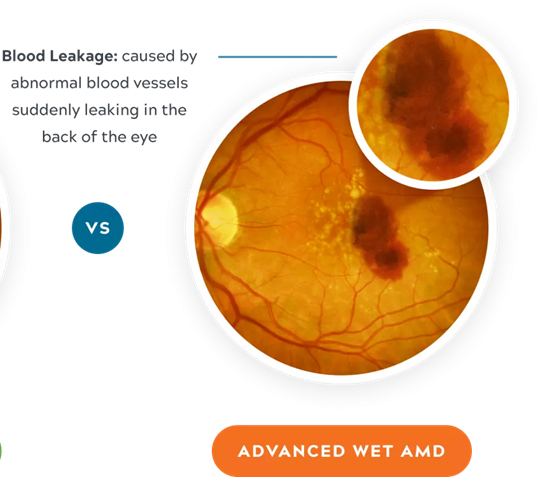
Retina with wet AMD
Image Courtesy of Foresee Home
Who is at Risk for AMD?
You are more likely to develop AMD if you eat a diet high in saturated fat (found in foods like meat, butter, and cheese), are overweight, smoke cigarettes, are over 50 years old, have hypertension (high blood pressure), or have a family history of AMD. Having heart disease is another risk factor for AMD, as is having high cholesterol levels. Caucasians (white people) also have an elevated risk of getting AMD.
What are the symptoms of AMD?
Many people with macular degeneration don’t have symptoms until the disease progresses.
You may experience:
- Being less able to see in low light.
- Worse or less clear vision. Your vision might be blurry, and it may be hard to read fine print, drive, or recognize faces.
- Problems or changes in the way you see colors.
- Straight lines that you see as curving or wavy.
- Blank spots or dark spots in your field of vision.
If you experience any of these symptoms, see an eye doctor as soon as possible.
How is AMD Diagnosed?
- During an eye exam, your ophthalmologist may ask you to look at an Amsler grid. This grid helps you notice any blurry, distorted, or blank spots in your field of vision.
- Your ophthalmologist will put dilating eye drops in your eye to widen your pupil. This allows them to look through a special lens at the inside of your eye to see if there are changes in the retina and macula.
- Optical coherence tomography (OCT) is another way to look closely at the retina. A machine scans the retina and provides very detailed images of the retina and macula.
- Your doctor may do fluorescein angiography to see what is happening with your retina. Yellow dye (called fluorescein) is injected into a vein, usually in your arm. The dye travels through your blood vessels. A special camera takes photos of the retina as the dye travels throughout its blood vessels. This shows if abnormal new blood vessels are growing under the retina.
- Optical coherence tomography angiography (OCTA) is another way to look closely at the blood vessels in and under the retina. This is like fluorescein angiography but does not use a dye.
How is AMD Treated?
Dry AMD Treatment:
Right now, only dry AMD with geographic atrophy can be treated. Two new medications are available: pegcetacoplan (Syfovre) and avacincaptad pegol (Izervay). These medications are injected into your eye, either monthly or every other month. Note that while these drugs can slow the development of geographic atrophy by about 14% to 20%, neither drug has demonstrated the ability to improve eyesight or restore lost vision. In addition, they may cause unwanted side effects, some of which can be severe.
There is no treatment for drusen. However, people with lots of drusen or serious vision loss might benefit from taking a certain combination of nutritional supplements. A large study (AREDS and the later AREDS 2 study) found people with drusen may slow their dry AMD by taking these vitamins and minerals daily: Vitamin C (500 mg), Vitamin E (400 IU), Lutein (10 mg), Zeaxanthin (2 mg), Zinc (80 mg), Copper (2 mg).
Your ophthalmologist can tell you if vitamins and minerals are recommended for your dry AMD, as not all forms will benefit from the AREDS supplements. Beta carotene should not be used by smokers as it raises the risk of lung cancer.
Wet AMD Treatment:
To help treat wet AMD, there are medications called anti-VEGF drugs. VEGF, which stands for vascular endothelial growth factor, is a protein that is important in the growth and development of new blood vessels. Anti-VEGF treatment helps reduce the number of abnormal blood vessels in your retina. It also slows any leaking from blood vessels. This medicine is delivered to your eye through a very slender needle. Anti-VEGF drugs must be injected every four to six weeks.
New drugs have emerged that require less frequent injections. In 2022, faricimab (Vabysmo) was approved for dosing up to every 4 months. Vabysmo inhibits two different factors involved in blood vessel formation, VEGF and angiopoietin-2. In 2023, the FDA approved a high-dose formulation of the anti-VEGF treatment aflibercept (Eylea HD) to be given every 2-4 months.
Laser surgery may also be used to treat some types of wet AMD. Your eye surgeon shines a laser light beam on the abnormal blood vessels. This reduces the number of vessels and slows their leaking.
Eye Healthy Foods:
Dark leafy greens, yellow fruits and vegetables, fish, and a balanced, nutrient-rich diet have been shown beneficial for people with AMD.
Talk with your ophthalmologist about ways to treat your AMD.
What Are Some Emerging Treatments for AMD?
Emerging Treatments for Wet AMD:
The primary drawback to anti-VEGF injections is that they must be given into the back of the eye every four to six weeks. Therefore, there has been a lot of research into new treatments that would be less onerous for patients.
Several combination therapies are in development that may increase treatment intervals. Two are in phase 3 trials and two are in phase 2 trials. One combination (foselutoclax-aflibercept) allowed 40% of patients to go 48 weeks without a supplemental injection and 64% to go treatment-free for more than 24 weeks. Another combination (umedaptanib pegol-aflibercept) halted disease progression in phase 2 trials, with “striking improvement” in previously untreated patients.
A host of novel drug delivery systems that could stretch out intervals between injections are now in human trials. In 2021, the FDA approved one such system, the refillable port delivery system (PDS) implant with the anti-VEGF drug ranibizumab (Susvimo). PDS is a small cylinder implanted into the eye and filled with ranibizumab, to be released for 6 months or so, then refilled in the physician’s office when it’s empty. New implants of PDS were halted in 2022 after the manufacturer, Genentech, received reports the device leaks, but Genentech says it has fixed those problems and confirmed the device should again become available for implants this year.
Several other novel drug delivery systems are in clinical trials. EYP-1901, which will start a phase 3 trial this year, is a depot that contains the drug vorolanib. The depot is inserted under the surface of the eye, where it biodegrades over 6 months as it releases the drug. An eye implant with the drug axitinib is also in phase 3 trials, and at least four implants, some of which biodegrade as they release the active ingredient, are in phase 1 or 2 trials.
Another promising new treatment for wet AMD involves retinal gene therapy as an alternative to monthly eye injections. An example is to employ the body to make its own anti-VEGF by inserting a harmless virus (called an adeno-associated virus/AAV) carrying the anti-VEGF gene into a person’s DNA. No fewer than 10 gene therapies are in phase 1 or 2 trials for AMD or another retinal disease called diabetic macular edema.
Emerging Treatments for Dry AMD:
Geographic atrophy is a robust area for drug development, according to David Boyer, MD, a retinal specialist in Los Angeles, CA. Based on a comprehensive review of pipeline programs, he found that no fewer than 16 investigative drugs are focusing on the condition. This is important as pegcetacoplan, the first FDA-approved treatment for geographic atrophy, has been associated with vision-threatening complications, as noted above.
Gene therapy is also being investigated for geographic atrophy. A phase 2b trial of JNJ-81201887, a soluble form of the C59 protein, a protective protein found in the cellular plasma membrane, started enrolling patients last year.
Oral tablets are another area of research for dry AMD. Four tablets are currently in clinical trials to treat geographic atrophy or early-stage dry AMD, including tinlarebant, which is in phase 3 trials for geographic atrophy.
Photobiomodulation (PBM) is a non-invasive therapy that has shown promise in sustaining vision and slowing the progression of dry AMD in clinical trials. It is suitable for patients with early to intermediate dry AMD. In patients with intermediate dry AMD, treatment with photobiomodulation (LumiThera) over a 2-year period showed visual acuity improvement and decreased the risk of progressing to wet AMD or geographic atrophy.
Finally, two drugs are in development that stabilize the membranes of mitochondria, parts of the cell that help us turn the energy we take from food into energy the cell can use. The drugs, called risuteganib (Allegro Ophthalmics) and elamipretide (Stealth BioTherapeutics), are both seemingly effective for improving vision in dry AMD and early-stage geographic atrophy. These drugs could be used in earlier stages of dry AMD than the recently approved drugs Syfovre and Izervay.
Sources:
Boyd, Kierstan. “What is macular degeneration?” American Academy of Ophthalmology, 13 Nov. 2023, www.aao.org/eye-health/diseases/amd-macular-degeneration
Wendt, Taylor. “What Is Geographic Atrophy?” WebMD, 22 Aug. 2022, www.webmd.com/eye-health/what-is-geographic-atrophy
Makumal, Reena. “What to know about Syfovre and Izervay for geographic atrophy.” American Academy of Ophthalmology, 18 Feb. 2024, https://www.aao.org/eye-health/tips-prevention/syfovre-izervay-geographic-atrophy-amd-macular-deg
“Macular Degeneration.” Cleveland Clinic, 14 Feb. 2023, https://my.clevelandclinic.org/health/diseases/15246-macular-degeneration
Compiled/edited by M. Kaplan, PhD, 5/2024.
Information Disclaimer: We do not recommend any particular treatment. Our Material might not represent all that is available on the subject. This information might not apply specifically to your own condition. Our Material is not intended as a substitute for medical care. Our Material should be used to formulate questions for discussion with your physician. We hope that the information you find at The Health Library will be useful in communicating with your health professionals. If you have any questions about your unique medical condition, we strongly advise that you see your physician.
